Gestational Diabetes: Symptoms, Risks, and Treatment During Pregnancy
Issue No. 4: Black Maternal Health
Words - Diana McDonnell, DNP
Illustration - Alexandra Folino
What is gestational diabetes?
Gestational diabetes occurs when diabetes is diagnosed in a pregnant person who did not have diabetes prior to pregnancy. Sometimes it’s temporary, lasting only for the duration of the pregnancy. However, it’s important to repeat testing after you give birth to make sure you no longer have diabetes after delivery.
What are the signs and symptoms of gestational diabetes?
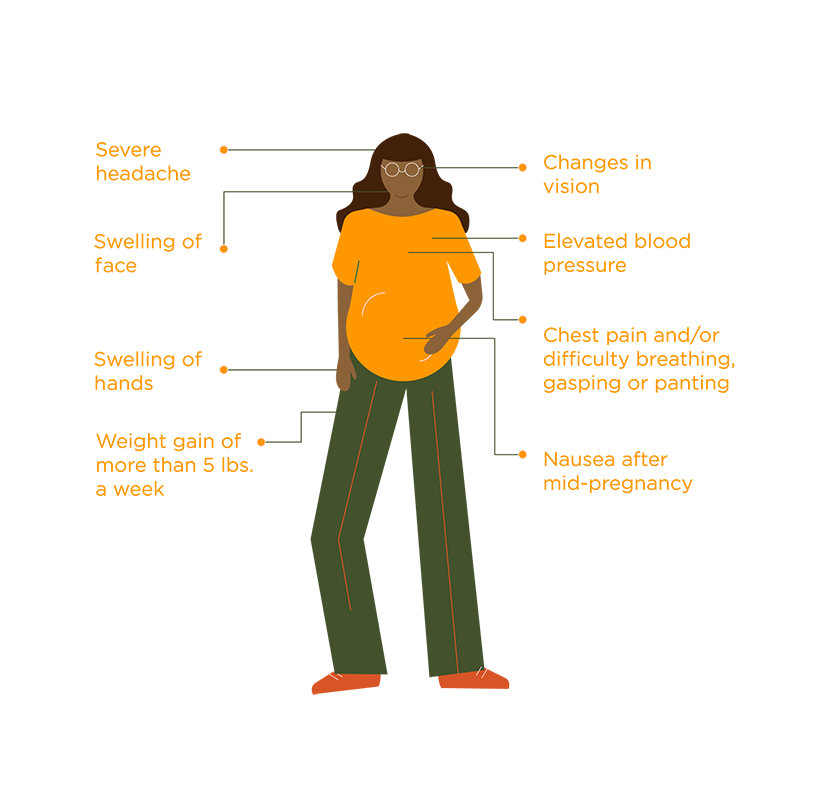
Some symptoms of gestational diabetes include:
Increased thirst
Frequent urination
Nausea
Fatigue
Blurred vision
Frequent infections
Blood in your urine
Contact your health care provider if you’re experiencing any of these symptoms. They could be symptoms of gestational diabetes.
Risk factors
You are more likely to develop gestational diabetes if you’re overweight or obese, over the age of 35, or have a family history of diabetes.
What are the long term complications of gestational diabetes?
If gestational diabetes goes undiagnosed or uncontrolled, it can cause problems for you and your baby. One possible result of gestational diabetes is a larger sized baby, which may mean delivery could require a C-section (surgical delivery). Gestational diabetes can also be associated with high blood pressure during pregnancy, which can create additional risks.
How can I prevent gestational diabetes?
Similar to type 2 diabetes, gestational diabetes can sometimes be controlled through exercise and eating healthy foods, but sometimes insulin is required for further management. If you have diabetes prior to becoming pregnant, you’ll need to check your blood sugar often to make sure it is at a safe level, and doesn’t become too high or too low.
Where can I find support for gestational diabetes?
The American Diabetes Association and the National Institute of Diabetes and Digestive and Kidney Diseases both have helpful information on managing gestational diabetes.